Gauteng Health Department trying to recover R4.6bn in unpaid patient fees
· Citizen
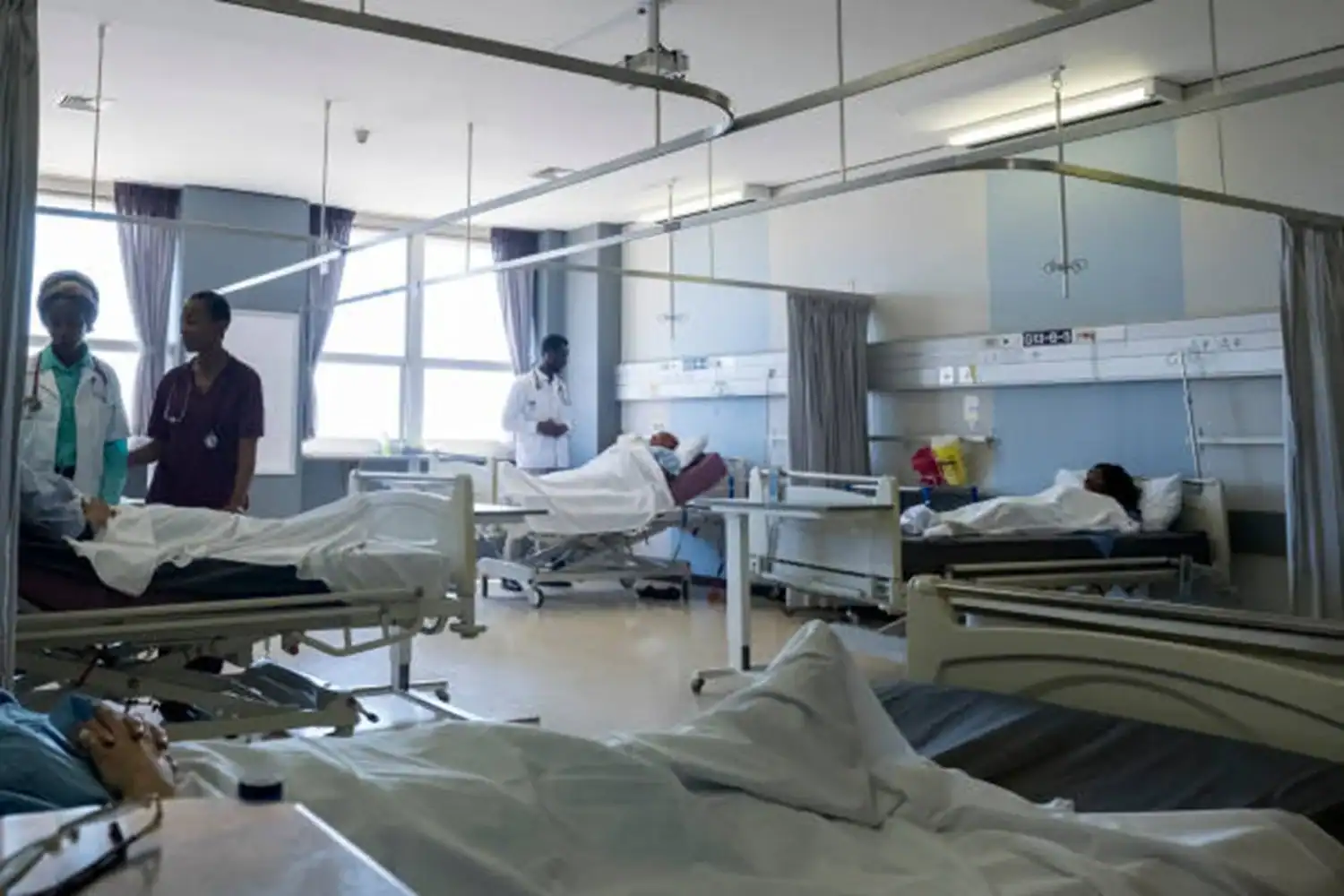
The Gauteng Health Department said it is trying to recover R4.6 billion in outstanding patient fees.
Visit mchezo.co.za for more information.
It reports that R2.6 billion of that portion is owed by self-paying patients – both South African citizens and foreign nationals.
The rest is owed by medical schemes and intergovernmental entities.
Unpaid fees
Speaking on Newzroom Afrika on Sunday, chief director of health economics and finance at the Gauteng Health Department, Siyabonga Jikwana, said recovering debt from patients is challenging for the department.
“Some of these patients, when they show up to these public institutions, they don’t have any form of identification.
“As a result, when we reach out to them for the payment, we don’t have any legal recourse for us to collect any of this revenue.
“While these constraints exist, the department continues to explore mechanisms, including bilateral engagements, where appropriate, to facilitate cost recovery,” said spokesperson Kealeboga Mohajane on Sunday in a statement.
The Road Accident Fund (RAF), the Department of Justice, South African Police Service (Saps), Correctional Services and other provincial governments also owe the department.
Debt collectors
The health department said it appointed five debt collectors in June 2025 to recover some of the debt.
As of 28 February, it said roughly R28.8 million has been recovered through these debt collectors.
“The department has strengthened its revenue collection capacity through participation in the Transversal Contract RT27-2024 for the provision of debt collection services to the State, managed by National Treasury,” said Mohajane.
This is managed by the National Treasury from 1 April 2024 to 31 March 2029.
Medical aid claims
She also said the department has introduced interventions to strengthen the manegement of medical aid claims.
“This includes tightening billing controls, improving claims submission processes and addressing longstanding administrative gaps that have historically resulted in delayed or disputed payments by medical schemes,” Mohajane said.
Stricter rules for patients
The department said it will be enforcing upfront payment protocols for patients who don’t qualify for free healthcare services in an attempt to limit the accumulation of new debt.
“In addition, measures to improve patient identification and verification systems are underway.
“These include integration with national databases to enhance traceability and support debt recovery efforts over time,” said Mohajane.
The constitution guarantees healthcare access, however, the National Health Act 61 of 2003 empowers state hospitals to apply a “means test”.
This process allows hospitals to categorise patients as full-paying, subsidised or free users based on their income levels.
“Despite these challenges, the department remains focused on strengthening internal systems, improving efficiency and maximising revenue collection within its legislative and operational mandate,” said Mohajane.